There are two main approaches in Prostate Biopsies : the transrectal prostate biopsy and the transperineal prostate biopsy. Both aim to collect prostate tissue samples for histopathological examination.
However, they differ significantly in needle pathway, infection risk, sampling accuracy, anesthesia requirements, and overall safety profile. Understanding Transperineal vs. Transrectal Prostate Biopsy is crucial for anyone preparing for a prostate biopsy procedure.
On this Page
Differentiate Transperineal vs. Transrectal Prostate Biopsy
When comparing transperineal vs. transrectal prostate biopsy, the biggest difference is infection risk. A transrectal prostate biopsy passes the needle through the rectum to reach the prostate. Because the rectum contains bacteria, there is a higher risk of infection, including urinary tract infection. Even with antibiotics, post-biopsy infections still occur with this method.
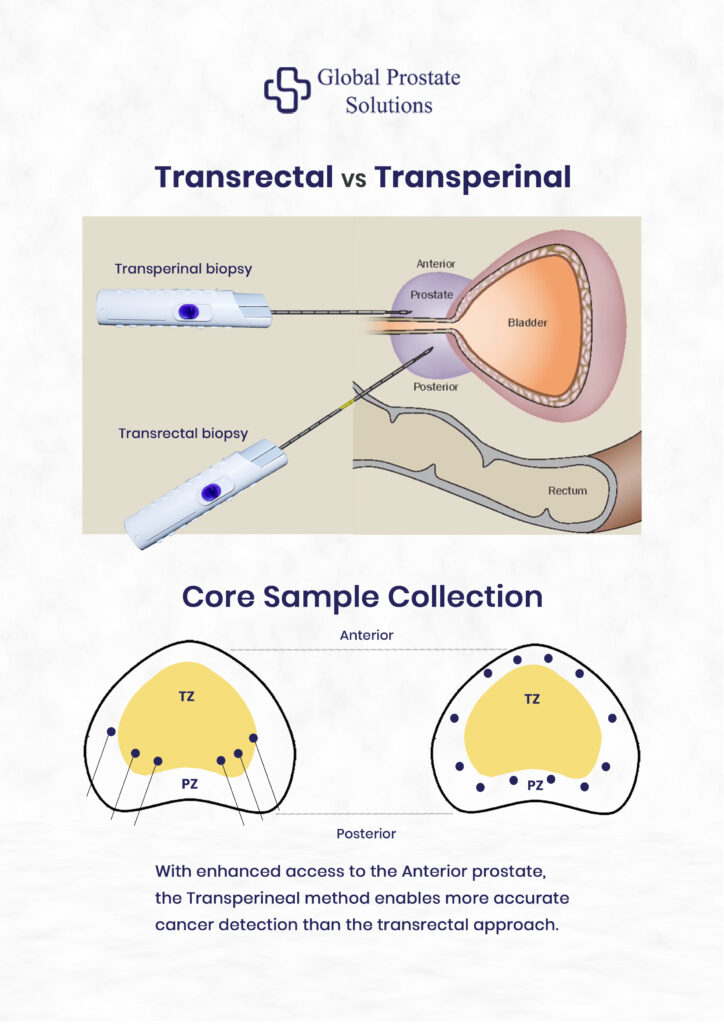
On the other hand, a transperineal prostate biopsy avoids the rectum completely. The needle enters through sterilized skin between the scrotum and anus. This significantly lowers the risk of infection. Large clinical studies have shown much lower rates of infectious complications with the transperineal approach compared to the transrectal method.
In terms of cancer detection, both techniques are effective. However, the transperineal approach may provide better access to certain areas of the prostate while offering improved safety. Let us understand the other differences too.
| Factor | Transperineal Prostate Biopsy | Transrectal Prostate Biopsy |
|---|---|---|
| Access Route | Through the perineum (skin between scrotum and anus) | Through the rectum |
| Infection Risk | Very low as minimal contact with rectal bacteria | Higher risk due to rectal bacteria exposure |
| Antibiotics Required | Minimal or sometimes none | Routine antibiotic prophylaxis required |
| Sepsis Risk | Significantly lower | Higher compared to TP |
| Cancer Detection (Anterior Zone) | Better access to anterior prostate | Limited access to anterior region |
| Anaesthesia | Often local or general (depending on setup) | Usually local anaesthesia |
| Hospital Stay | Day-case procedure | Day-case procedure |
| Procedure Time | Slightly longer (in some setups) | Generally quicker |
| Patient Recovery | Mild perineal discomfort possible | Rectal discomfort, minor bleeding possible |
| Current NHS Trend | Increasingly preferred method | Gradually being replaced by Transperineal |
What is a Transrectal Prostate Biopsy?
The transrectal ultrasound-guided prostate biopsy (TRUS biopsy) has been the standard technique for decades. In this procedure, biopsy needles are inserted through the rectal wall into the prostate gland using real-time ultrasound imaging for guidance. The prostate sits directly in front of the rectum, which makes this pathway technically convenient.
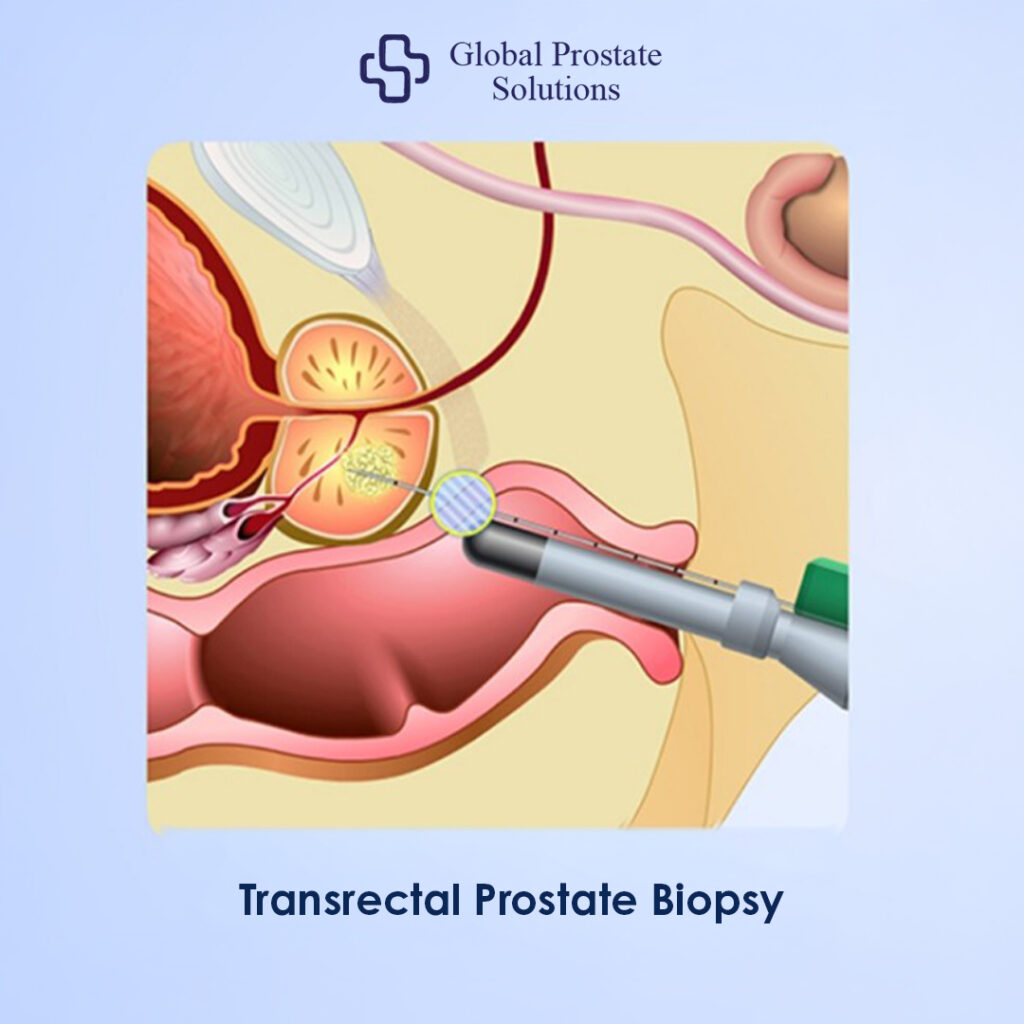
During the procedure, an ultrasound probe is inserted into the rectum to visualize the gland. After administering local anesthesia, a spring-loaded biopsy gun collects multiple tissue cores, typically 10 to 12 samples in a systematic pattern.
The procedure is usually completed within 15 to 20 minutes and is performed as an outpatient procedure. Some technical aspects of TRUS biopsies are;
- Performed under local anesthesia
- Uses systematic core sampling
- May incorporate MRI fusion targeting
- Needle passes through the rectal mucosa
- Requires antibiotic prophylaxis
Although efficient and widely available, the transrectal biopsy carries one important limitation: the rectum contains a high bacterial load.
What is a Transperineal Prostate Biopsy?
The transperineal prostate biopsy represents a significant evolution in prostate cancer diagnostics. Instead of passing through the rectum, the biopsy needle enters the prostate through the perineal skin, the area between the scrotum and the anus. The rectum is not breached. This single anatomical difference dramatically reduces the risk of infectious complications.
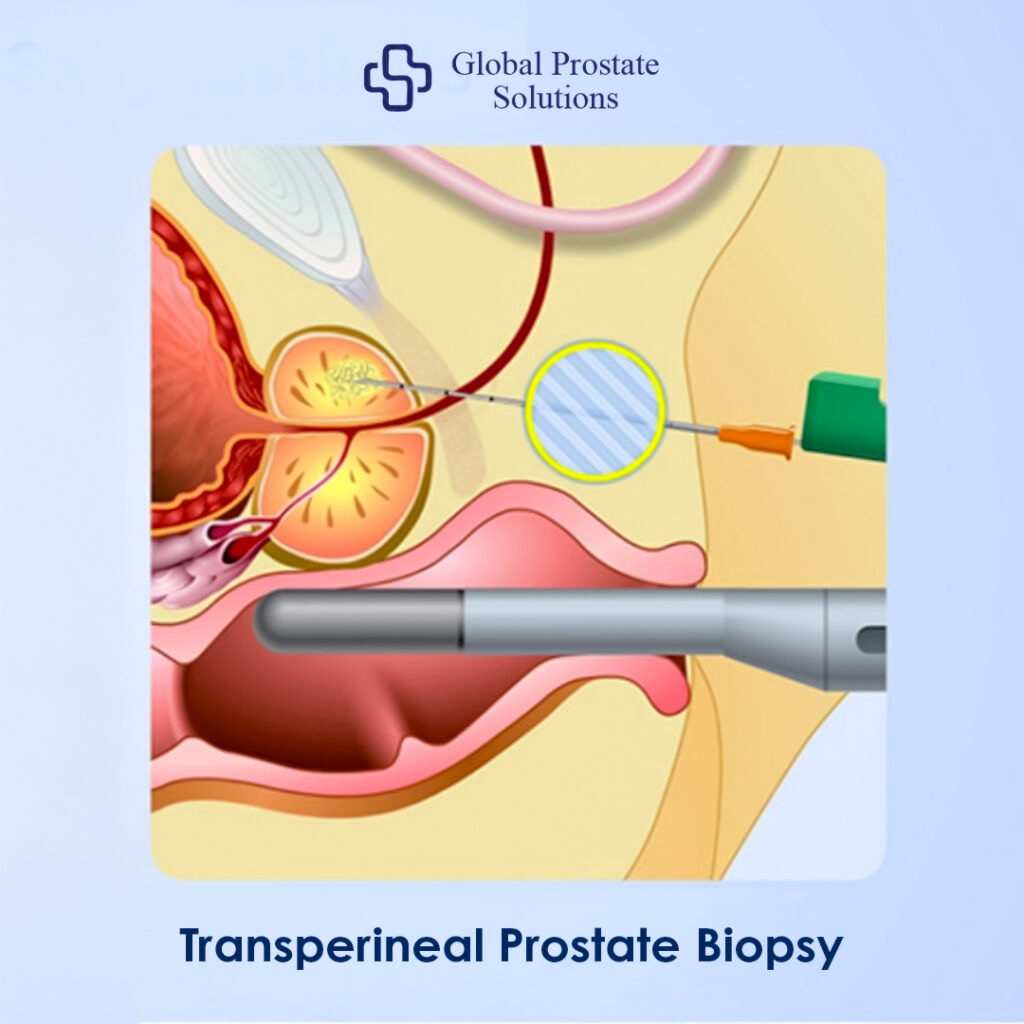
In a transperineal biopsy procedure, the patient lies on their back. The perineal area is carefully sterilised. Local anesthesia or light sedation is administered. An ultrasound probe may still be inserted into the rectum for imaging guidance, but the biopsy needle passes through disinfected perineal skin using freehand technique.
Which have the accurate detection rates in prostate biopsy?
Both transrectal and transperineal prostate biopsy techniques are effective in diagnosing prostate cancer. However, studies suggest that transperineal biopsy may improve the detection of clinically significant prostate cancer, particularly in anterior lesions.

Demanding Prostate Biopsy Kit
in the United Kingdom.!!!
Which Prostate Biopsy method is safer?
When comparing transperineal vs. transrectal prostate biopsy, infection risk is the key difference. From a safety standpoint, the transperineal prostate biopsy is considered safer because it carries a significantly lower risk of sepsis. Since the needle does not pass through the rectum, exposure to bacteria is minimized.
With rising global antibiotic resistance, many urology centers are now shifting toward the transperineal technique as the preferred diagnostic approach. In the debate of transperineal vs. transrectal, the best biopsy method still depends on several factors:
- Patient health status
- Individual infection risk factors
- MRI findings
- Prior biopsy history
- Urologist experience
Conclusion
A prostate biopsy is essential for confirming prostate cancer. While both methods work well, the discussion around transperineal vs. transrectal biopsy increasingly favors the transperineal approach due to its lower infection risk and strong diagnostic accuracy.
If you need a biopsy, speak with the best urology consultant in Manchester about the technique being used and what to expect. Understanding your options helps you make safer, more confident decisions about your care.
FAQs
1. What is the difference between transperineal and transrectal?
The main difference in transperineal vs transrectal prostate biopsy is the needle pathway. A transrectal biopsy passes through the rectum, while a transperineal biopsy enters through the skin between the scrotum and anus. The transperineal approach has a lower risk of infection because it avoids rectal bacteria.
2. Which is more painful, transrectal or transperineal prostate biopsy?
Both procedures are generally well tolerated. Transrectal biopsy may cause brief rectal pressure, while transperineal biopsy can cause mild soreness in the perineal area. With proper anesthesia, pain is usually minimal in both methods.
3. What is the difference between a transrectal and a transperineal biopsy?
TRUS (Transrectal Ultrasound-guided biopsy) is a transrectal procedure where the needle passes through the rectum using ultrasound guidance. A transperineal biopsy also uses ultrasound, but inserts the needle through the perineal skin instead. The key difference is the route used to reach the prostate.
4. What is the safest type of prostate biopsy?
From an infection standpoint, the transperineal prostate biopsy is considered the safest. It avoids the rectum and has a significantly lower risk of sepsis compared to the transrectal method.
5. How long does it take to recover from a transperineal biopsy?
Most men recover within 24 to 48 hours after a transperineal biopsy. Mild soreness or blood in the urine may occur, but usually resolves quickly. Normal activities can typically resume within a couple of days.




